You can now self-refer as soon as you know that you are pregnant by phoning or texting the the maternity unit. Telling us promptly will ensure you receive maternity care that takes into account all your health needs and preferences.
The first appointment with a midwife will take place either at the hospital or at your GP surgery.
You will be offered several antenatal screening tests which are performed on a sample of your blood. For more information please click here.
To make sure you are given the support you need and so that any risks are spotted early, your midwife will also ask you a few questions. You too may have lots of questions to ask us.
We look forward to seeing you soon.
The maternity team
Lewis Maternity team: 01851 708301 text: 07769932189
Uist Midwives: 01870 603354
Barra Midwives: 01871 810665
From your booking appointment your midwife will be able to tell you if you are a low risk pregnancy or a high risk pregnancy based on what you have told us. She will explain the reasoning to you.
Screening tests – there are a wide range of tests on offer to you. Please click here for more details
You will be offered screening tests for you and your baby. This is in accordance with the UK National Screening Committee guidelines.
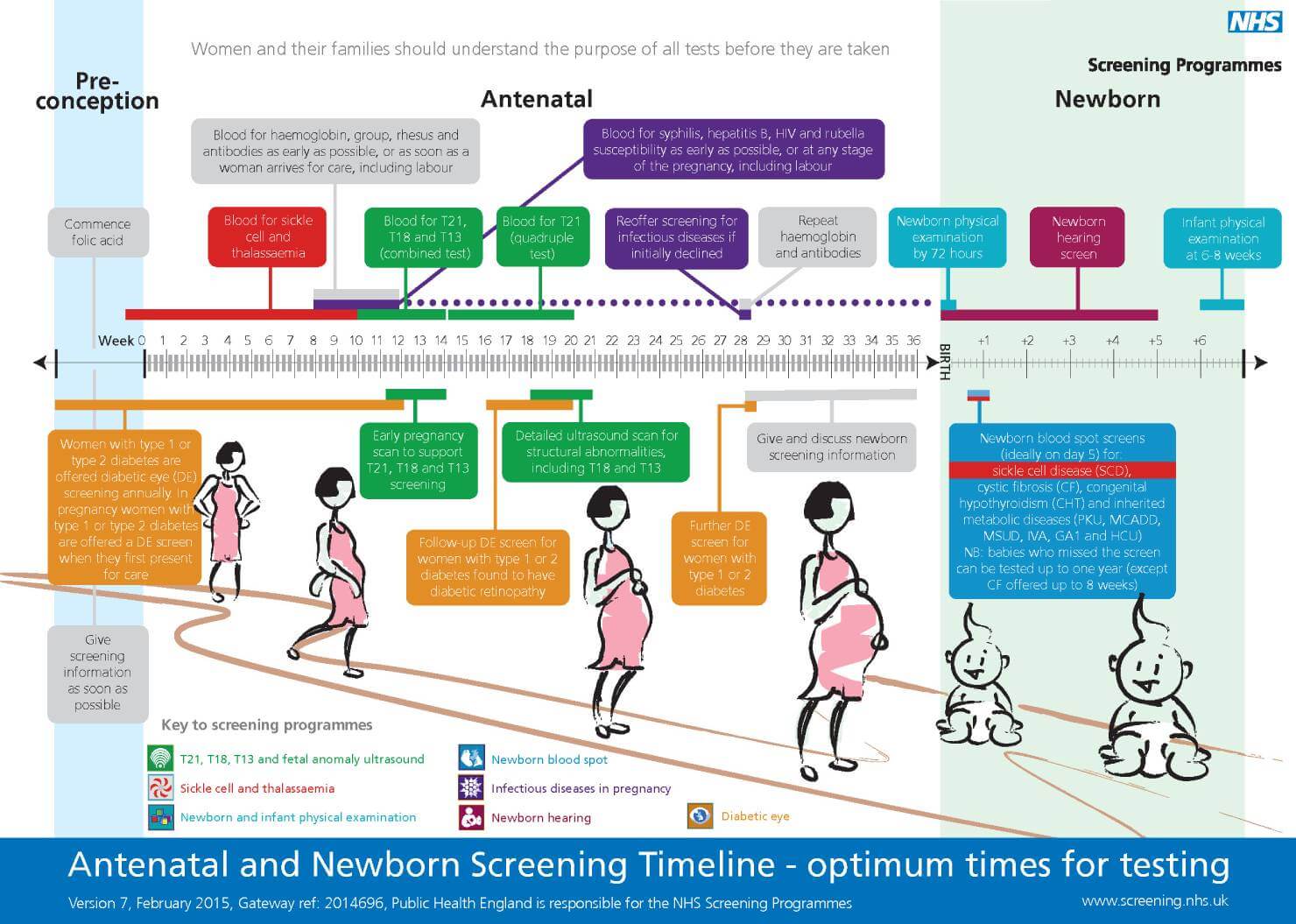
It is important that you read the booklet and inform your midwife of any relevant conditions that may occur in you, your partner or your immediate families.
More Information about screening tests:
Ultrasounds Scans
You will be routinely offered two scans during your pregnancy. The first scan is offered between 11+0 and 13+6 weeks of the pregnancy and the purpose of this scan is to:
- Measure the length of your baby, to check that it correlates with your dates and
estimate an expected due date - Check your baby’s heart rate
- Check if there are multiple pregnancies – twins or more
- Check for abnormalities
- Offer you screening for Down's syndrome
The second scan offered is between 18+0 – 20+6 weeks of the pregnancy and the purpose of this scan is to:
- Look at all the major organs and limbs to detect any structural abnormality with
the baby - Determine where the placenta has embedded
- Determine the amount of amniotic fluid
In some pregnancies your Obstetrician will recommened additional scans.
Blood Tests
You will be offered a number of blood tests at your booking appointment, which we encourage you to have. Blood tests are a vital way of checking your and your baby’s health and we can provide the correct treatment for you and your baby if any of the results were to show you or your baby were at risk, or affected.
- Screen for haemoglobinopathies (blood disease) – to see if you are a carrier
of Sickle cell or Beta Thalassemia - Screen for infectious diseases – Hepatitis B, HIV, Syphilis and whether you
are immune to Rubella or not - Determine your blood group and rhesus factor
Screening for Down's Syndrome
You will be offered screening for Down's Syndrome following your first scan. The screening test is able to provide specific information about your chance of having a baby affected with Down's Syndrome. The ‘Combined test' (CUBS) is offered to all women under 14+1 weeks of pregnancy and involves measuring three markers in relation to the pregnancy. The markers are:
- Measurement of fluid under the skin at the back of the baby's neck, known as the nuchal translucency (NT).
- Measurement of two serum markers found in the mother's blood from the pregnancy.
The results from all of these markers are processed by a very specific computer programme to generate a ‘risk' or your chance of having a baby with Down's Syndrome. Any number that is below 1 in 150 means that there is a higher chance of the baby having Down's Syndrome and you will be offered further testing, if you wish. Numbers that are above 1 in 150, means that there is a lower chance of the baby having Down's Syndrome. However, it has to be remembered that a screening test cannot diagnose Down's Syndrome. If the result is ‘high' the screening midwives will contact you to discuss the implications of the result and your options.
 We offer classes in the maternity unit from when you are around 28-32 weeks pregnant. An invitation letter will be sent to you.
We offer classes in the maternity unit from when you are around 28-32 weeks pregnant. An invitation letter will be sent to you.
Why go to classes?
Parentcraft classes can help you to prepare for your baby's birth and learn to look after and feed your baby. You can learn about the different arrangements for labour and birth, and the choices available to you. This can help you to make your own birth plan.
Knowing the health benefits of breastfeeding can help you make an informed choice in how you decide to feed your baby. At classes you can gain information and practical skills that will help you be successful in your chosen method of feeding.
You will be able to discuss your plans and any worries with a midwife and with other parents. Classes are also a good way to make friends with other parents who are expecting babies around the same time as you. These friendships often help parents through the first few months with a baby. If you have any questions about this then please ask your midwife at your next appointment.
Women who require close observation during their pregnancy, or require inpatient induction of their labour are admitted to this area in the Western Isles Hospital. Women in Uist and Barra will sometimes need cared for here also and this plan of care would be arranged accordingly between midwifery teams.
A team of midwives and an obstetrician will care for you and ensure you have an individualised plan for your stay.
Facilities
- 2 single rooms
- 2 bays with 3 beds and en-suite
Visiting times:
- Open visiting for partners only
- 14:30 – 16:30 all other visitors
- 18:30-20:30
Meals are available for mothers and special dietary requirements can be accommodated. Self service breakfast, lunch 12.30pm, dinner 5:30pm.
Alcohol in Pregnancy
It is best to avoid alcohol completely during pregnancy, as any alcohol you drink while pregnant will reach your baby and may cause harm. Women who are trying to conceive should also avoid drinking alcohol. There is no ‘safe' time for drinking alcohol during your pregnancy and there is no ‘safe' limit. We do know that the risk of damage increases the more you drink, but there is no cut-off level at which damage is known to occur. Drinking no alcohol during your pregnancy is the best and safest choice. Everyone has a role to play in supporting pregnant women to avoid alcohol, and pregnancy is an ideal time for partners to cut down on their drinking too.
Fetal Alcohol Spectrum Disorders
Regularly drinking and binge drinking in pregnancy can lead to an increased risk of a wide range of development issues and physical disabilities including Fetal Alcohol Spectrum Disorders (FASD). Although children with FASD look healthy, the effects can include physical, mental, behavioural and learning disabilities.
One particular disorder in FASD is Fetal Alcohol Syndrome (FAS). Children with FAS have restricted growth, distinctive facial features including small eyes and a flat area between the nose and upper lip, and lifelong learning and behavioural problems.
If you have any concerns, your midwife, GP or other healthcare staff will be happy to discuss these with you.
Smoking and the unborn baby
Protecting your baby from tobacco smoke is one of the best things you can do to give your child a healthy start in life. It's never too late to stop smoking. Every cigarette you smoke contains over 4,000 chemicals, so smoking when you are pregnant harms your unborn baby. Cigarettes can restrict the essential oxygen supply to your baby, so their heart has to beat harder every time you smoke.
Benefits of stopping smoking in pregnancy
Stopping smoking will benefit both you and your baby immediately. Harmful gases like carbon monoxide and other damaging chemicals will clear from your body. When you stop smoking:
- you will have fewer complications in pregnancy
- you are more likely to have a healthier pregnancy and a healthier baby
- you will reduce the risk of stillbirth
- you will cope better with the birth
- your baby is less likely to be born too early and have to face the additional breathing, feeding and health problems that often go with being premature
- your baby is less likely to be born underweight: babies of women who smoke are, on average, 200g (about 8oz) lighter than other babies, which can cause problems during and after labour, for example they are more likely to have a problem keeping warm and are more prone to infection
- you will reduce the risk of cot death, also called sudden infant death.
Stopping smoking will also benefit your baby later in life. Children whose parents smoke are more likely to suffer from asthma and other more serious illnesses that may need hospital treatment.
The sooner you stop smoking, the better. But even if you stop in the last few weeks of your pregnancy this will benefit you and your baby.
Second-hand (passive) smoke harms your baby
If your partner or anyone else who lives with you smokes, their smoke can affect you and the baby both before and after birth. You may also find it more difficult to stop if someone around you smokes.
Second-hand smoke can also reduce birth weight and increase the risk of cot death. Babies whose parents smoke are more likely to be admitted to hospital for bronchitis and pneumonia during the first year of life. http://www.maternal-and-early-years.org.uk/second-hand-smoke
Nicotine replacement therapy (NRT)
You can use NRT during pregnancy if it will help you stop smoking, and you're unable to so without it. It's not recommended that you take stop smoking tablets such as Champix or Zyban during pregnancy.
NRT is available as:
- patches
- gum
- an inhalator
- nasal spray
- mouth spray
- lozenges
- microtabs
Before using any of these products, speak to your midwife, GP, a pharmacist or a specialist stop smoking adviser for more detailed information and support.
Quit Your Way Hebrides
To find out more about quitting and to get support, you or your partner can call Quit Your Way Hebrides, your local stop smoking service in the Western Isles. Or, if you prefer, ask your midwife or doctor to refer you.
Quit Your Way Hebrides offers a team of highly trained support workers who will be delighted to support you in your quit attempt.
You can contact them for free, friendly, confidential support on:
Quit Your Way Hebrides – Western Isles
Block 11, Laxdale Court, Stornoway, Isle of Lewis, HS2 0GS
Tel. 01851 701623 / 762018 or 762019
Email: wi.hebridesquityourway@nhs.scot
Quit Your Way Hebrides has advisors across the Western Isles, please call and we will be happy to put you through to your local advisor.
Please give Quit Your Way Hebrides a call, it is much easier to quit than you may realise.
- NEXT PAGE: Maternity Services - Giving Birth
- LAST REVIEWED ON: January 22, 2021